Managing Skin Flare-Ups During Peri-Menopause
- Kirsty Lakstins-Adams
- Jan 21
- 3 min read
Updated: Feb 17
Understanding Peri-Menopause
Perimenopause is the transitional phase that usually occurs 2 to 12 years before menopause. This period is often marked by significant hormonal shifts and an array of symptoms. Menopause is defined as the point one year after your last period, typically associated with fewer symptoms.
During peri-menopause, fluctuating estrogen levels and reduced progesterone can lead to a range of symptoms, including:
Longer, heavier periods
Shorter cycles or missed periods
Sore and lumpy breasts
Interrupted sleep patterns
Night sweats
Increased migraine headaches
Heightened PMS symptoms, including mood swings
Unexplained weight gain, sometimes as high as 10% of body weight, especially around the mid-region
Some other symptoms that might not seem related are itchy ears, crawling skin, joint pain, lowered immunity, increased cholesterol, and blood sugars
These symptoms can feel overwhelming, especially for women experiencing skin conditions like psoriasis, rosacea and eczema.
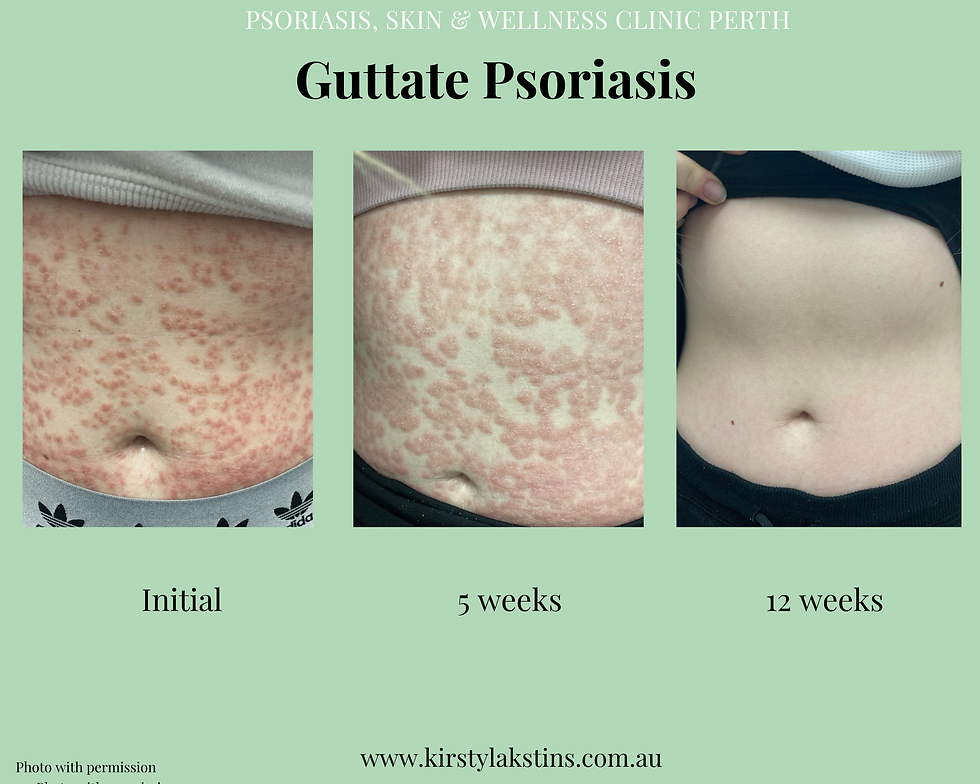
What is Psoriasis?
Psoriasis is a chronic autoimmune skin condition that speeds up the growth cycle of skin cells. This results in thick, red, scaly patches that often appear on areas such as elbows, knees, scalp, and lower back. About 2% to 3% of the population is estimated to be affected by psoriasis, and it often goes hand-in-hand with other health issues, like psoriatic arthritis, blood sugar issues, high blood pressure, as well as stress or depression.
How Hormonal Changes Affect the Skin
Hormonal shifts during peri-menopause can have a significant impact on skin health.
Hormonal Changes
Fluctuating estrogen levels can worsen skin conditions like psoriasis. Just as hormone levels change during adolescence and pregnancy, the shifts during peri-menopause can trigger flare-ups in women already prone to skin issues. Welcome to puberty all over again.
Immune System Factors
The immune system plays a key role in psoriasis. External factors, such as infections (like influenza or strep throat), can trigger immune responses, leading to flare-ups. Additionally, women with autoimmune conditions, such as Hashimoto’s thyroiditis, may see worsening psoriasis symptoms during this time.
Medication Side Effects
Some medications, including certain antidepressants and blood pressure medications, can aggravate psoriasis. If you suspect your medication is affecting your skin, talk to your doctor about alternatives.
Blood Sugar Fluctuations
Blood sugar levels often fluctuate during peri-menopause, increasing risks of insulin resistance. Studies show that maintaining stable blood sugar can help manage psoriasis symptoms. Consider dietary changes—like incorporating more whole grains and lean proteins while decreasing processed sugars and alcohol.
Taking Control: Effective Strategies
Managing skin flare-ups like psoriasis during peri-menopause requires a holistic approach that addresses both hormonal balance and skin health. Here are some actionable steps:
Hormonal Balance
Consult your GP: Speak to your doctor about hormonal changes. Hormone replacement therapy (HRT) helps some women reduce symptoms linked to fluctuations in hormone levels. Getting some blood or urine testing done to see what changes are occurring may be beneficial.
Embrace Lifestyle Changes: Regular exercise can boost mood and support hormone regulation. This may involve changing the type of exercises you are doing. Practicing stress-reducing techniques like yoga or meditation can help with joint pain and improve sleep.
Track Symptoms: Use a symptom diary to identify patterns and triggers related to both hormonal and skin changes.
Skin Care
Hydrate: Keeping your skin well-hydrated is vital. Use moisturisers specifically designed for psoriasis to alleviate dryness and scaling.
Consult your naturopath: At the clinic, we can recommend tailored treatments, ranging from topical creams to supplements. This personalised approach can significantly improve skin health.
Avoid Triggers: Identify irritants such as harsh soaps and certain fabrics that could make psoriasis worse. Dietary triggers such as high sugars, caffeine, alcohol, and processed foods can all exacerbate skin conditions.
Stress Management: Since stress often exacerbates psoriasis, include relaxation techniques, like deep-breathing exercises or journaling, into your routine.

Embracing Your Journey
Navigating the peri-menopause rollercoaster can feel overwhelming, especially with skin flare-ups like psoriasis, acne, rosacea, or eczema added to the changes. Understanding the causes behind these changes—like hormonal fluctuations, immune responses, and lifestyle factors—empowers women to take charge.
By working with a naturopath, committing to lifestyle adjustments, and implementing effective skincare routines, you can manage this challenging phase with confidence. Remember, you are not alone; many women are dealing with similar struggles and finding ways to cope—one day at a time.

Take each step of this journey thoughtfully and embrace the hope of better days ahead!
In health & happiness,
Kirsty

Comments